Suffering from sleeplessness? Let’s examine if red light could be your key to fighting back and getting a good night’s sleep. (Please note: the purpose of this blog post is purely educational; it is not meant to diagnose, prevent, or cure any disease. Always consult your doctor before starting any form of medical treatment.)
One in every two or three people worldwide deal with insomnia, and these numbers have spiked after the pandemic. Even though it is a common problem, chronic insomnia can lead to serious consequences. I know— not exactly what you want to hear when you’re already anxious about getting enough sleep before work tomorrow. Since we’re both awake right now, let’s explore what insomnia is; and for the love of everything good, how do you cure it?

Contrary to what you may have been told, most adults need seven to eight hours of sleep every night. Anything less than that, and you’ll suffer from irritability and difficulty concentrating, which can lead to mistakes at work or rear-ending someone in a parking lot. Over the long term, sleep deprivation can bring on memory problems and lowered immune system function. These issues can wreak havoc in all areas of your life, from relationships to work to basic health. If you’re one out of every five adults living with mental illness in the US, sleeplessness can make existing symptoms worse, or even trigger an episode.
What Is Insomnia?
Everybody experiences difficulty falling or staying asleep sometimes. Noisy neighbors, snoring partners, and small children can all make it hard to catch those sweet, sweet ZZZ’s. Sleepless nights become insomnia when, over time, you can’t sleep even if nothing’s stopping you, and your sleeplessness affects your ability to function the next day.
Insomnia Symptoms
- Trouble falling asleep at night
- i.e. lying awake in bed for more than 30 minutes trying to fall asleep
- Trouble staying asleep at night
- e.g. waking up multiple times per night, or waking up and being unable to fall asleep again for more than 30 minutes
- Waking up too early but being unable to go back to sleep
- Feeling exhausted even after a full night’s sleep
- Daytime sleepiness
- Anxiety about sleeping
Understandably, human beings have tried everything to cure sleeplessness. And I mean everything. Ancient Egyptians drank psychoactive latex made from wild lettuce, and the Romans got creative with rodents. Modern insomniacs try melatonin, Benadryl, and meditation instead of soaking our feet in doormouse fat, but each to their own. What ultimately treats your insomnia depends, in part, on what’s causing it.
Acute vs. Chronic Insomnia
There are two main types of insomnia: acute and chronic. Acute insomnia is difficulty sleeping in response to a specific trigger such as stress or an upsetting event, and usually goes away within a few days or a few weeks. Insomnia becomes chronic if it lasts longer than a month. Chronic insomnia may be the result of ongoing stress, a medical condition such as heart disease or depression, or simply bad sleep hygiene (like scrolling on Instagram for an hour before bed). Certain medications, or neurodiversity like ADHD, can also cause chronic insomnia.

Hilariously, and by hilariously I mean not at all, chronic insomnia can be caused by several factors at once. If you have sleep apnea and stress and ADHD and heart disease and depression, treating your lack of sleep may be like playing Whack-a-mole. Insomnia can also be its own condition (called primary insomnia), meaning it’s not a side effect of something else.
When should you see a doctor for insomnia?
As soon as sleeplessness starts affecting your daily life, you should go to the doctor. Yes, really. No, it’s not stupid. Insomnia can lead to traffic accidents or even be a symptom of an undiagnosed medical problem, so you should definitely seek medical advice and support.
Seasonal Affective Disorder and Insomnia
The changing of the seasons, particularly warm to cold, can also cause insomnia, along with a feeling of listlessness, apathy, and depression. Commonly called “the winter blues”, about 10 million US Americans live with Seasonal Affective Disorder. Despite the unbelievably on-the-nose acronym, SAD can be a serious ailment and often requires medical treatment. Someone with SAD may experience some or all of the following symptoms:
SAD Symptoms
- Trouble sleeping
- Oversleeping
- Low energy
- Feeling sluggish
- Loss of interest in activities previously enjoyed
- Feeling sad or down most of the time, for days on end
- Appetite changes, especially either craving carbs or else loss of appetite.
- Changes in weight
- Difficulty concentrating
- Feeling hopeless, anxious, guilty, agitated, and/or worthless
- Having thoughts about not wanting to live
If you are in emotional distress or thinking about your own death, please know you are not alone. Talk to a trusted friend or family member, and/or your doctor or another medical professional about what you’re experiencing. In the US, help is also available 24/7 at the Suicide and Crisis Lifeline. Dial 988 to speak with someone in either English or Spanish. You do not have to be actively suicidal to talk to a counselor; anyone in emotional distress can call this number to talk with a caring, trained listener even if you only want a sympathetic ear.

SAD is frequently caused by a lack of sunlight and is especially common in people who live far from the equator, where winter means fewer daylight hours. Many people don’t know they have SAD– including yours truly, who is trying very hard not to make SAD puns. I live in sunny California, but work from home in a neighborhood that isn’t walkable. In October 2022, I started feeling sluggish and sleepy no matter how much coffee I drank. In a matter of days, I was so tired that I gave up writing books in the evenings and instead started spending my off-hours melting into a lump on my couch binge-watching River Monsters.
I did some research into possible causes for my energy nosedive. SAD seemed to explain my symptoms and appeared easy to treat at home, so I thought I’d save money on doctor’s visits and test myself. I already took vitamin D daily, but what else could I do? I bought a bright sun lamp and sat under it for 20 min every morning. After a couple of days, my energy spiked up again and I felt like myself. The sun lamp’s bright light simulates morning rays, which causes the skin to produce vitamin D and the brain to produce important hormones like serotonin. Early sunlight also helps reset the circadian rhythm, solving some incidents of insomnia. Problem solved?
Well… yes. One of them. I catch up on emails under a bright light to keep my energy high during the winter, but that didn’t solve my insomnia. See, I have chronic, primary insomnia.
Treating Primary Insomnia
My symptoms first appeared as a teenager, when I lay awake in bed for hours, night after night, but for some reason couldn’t fall asleep. I didn’t have a name for my problem and didn’t tell anyone about it. Young Me figured that, if I had to go to school even though I didn’t want to, it wasn’t unthinkable that I couldn’t sleep even if I did want to.
Sometimes I could pinpoint what caused my sleep problems— namely, 100℉ summers in California’s Central Valley, with no air conditioning. During those broiling summer nights, Young Me dragged a towel into the hallway, plopped a fan in front of it, and lay on the towel in my pajamas, struggling to sleep.
The problem got worse in my twenties. Every so often, for about two weeks at a time, I’d spend hours trying to fall asleep. I have a gold medal in memory problems from the funhouse of trying to read while chronically sleep-deprived. My memory at the time was so bad that I got caught in an infinite loop rereading the same sentence, since by the time I finished it I couldn’t remember how it started, so I had to go back and look, and then I forgot how it ended. (Do not recommend.)
Family and friends suggested a variety of over-the-counter and prescription sleep aids. I tried them all. Benadryl, melatonin, and one doctor’s prescriptions worked for a while, but my body adapted to each of them pretty fast and I didn’t want to keep upping the dosage to knock myself out, so, days or weeks after I started one, I had to give up.
Ambien was one medication that worked consistently, but for some reason it made my dreams so unbearably boring I couldn’t stand taking it. “Boring?” I hear you cry. “You stopped taking an effective sleep aid because your dreams were boring?” Yeah. Spend a month driving your truck down a quiet road eight hours a night, every night, and you’ll want off that ride, too.
Many people can take Ambien without getting bored out of their skull, but if you and your doctor are considering this medication they should talk to you about its risks. While Ambien is an effective sleep aid, it can also be addictive and sometimes cause behavioral changes like suicidal ideation.
My insomnia came and went as it pleased, bringing noticeable exhaustion and lack of creativity that affected my hobbies. I finally spoke to another doctor, who prescribed sleep hygiene. Sleep hygiene means creating the best possible environment for sleep: have a consistent bedtime, no caffeine or stimulating electronics for several hours before bed, exercise during the day, and make sure your bedroom is quiet, dark, and comfortable. However, I already did all these things and I still couldn’t sleep.
I tried everything else I could think of: hot baths and chamomile tea, guided sleep meditations, rereading familiar books. Nothing worked, or at least not for long. Then, a colleague suggested Photobiomodulation for my insomnia. Photo-what now? Photobiomodulation, or red light therapy, is a form of low-light therapy used to treat pain and promote wound healing. The medical field is exploring red light therapy as a treatment for various ailments, from arthritis to cancer to insomnia.

Before jumping in and trying light therapy as a potential treatment, I had to ask: would it be possible for red light therapy to cause (or worsen) insomnia?
Can Red Light Therapy Cause Insomnia?
Our bodies have a natural sleep-wake cycle called the circadian rhythm. It’s fine-tuned to suppress or produce melatonin based on ambient light levels. Bright light keeps us awake; low light helps us go to sleep. Most people have a circadian rhythm that follows the 24-hour day, taking cues from the sun to make us more alert or groggy. Blue light from phones, TVs, and tablets mimic daylight, which tricks our circadian rhythm into thinking it’s time to be awake. (That’s why you’re supposed to avoid screen time before bed.)
Blue light is so effective at waking us up that it’s already used to treat insomnia by resetting the circadian rhythm. People struggling with Delayed Sleep Phase Disorder (DSPD) have an internal clock set about two hours later than what is considered socially acceptable. Someone with DSPD may not feel sleepy until around midnight, even if they’re tired, because their circadian rhythm is still producing “awake” signals. In the morning, someone with DSPD may struggle to wake up earlier than around 10 o’clock because their brain is still producing “sleep” signals.

In this case, using a device that emits bright white light first thing in the morning, like a sun lamp, can trigger alertness earlier in the day— which will bring on sleepiness sooner than their internal clock would otherwise allow. (Note that DSPD is not the same as being a night owl. Night owls stay up late because they like doing so, while someone with DSPD wants to sleep and can’t.)
Similarly, offices that have bright natural light can prevent the typical post-lunch slump in employees’ energy levels. Whether you deal with DSPD or not, soaking in plenty of bright natural light during the day will keep your circadian rhythm on track. But if blue and white light keep people awake, what about red light? The answer is in the wavelengths.
Light functions in part as a wave, and it turns out that exposure to different wavelengths has different effects on melatonin production. Full spectrum light, or white light, keeps you awake, and so do short wavelengths between 435 – 445 nanometers (nm)— blue light— which suppress melatonin to keep you alert.
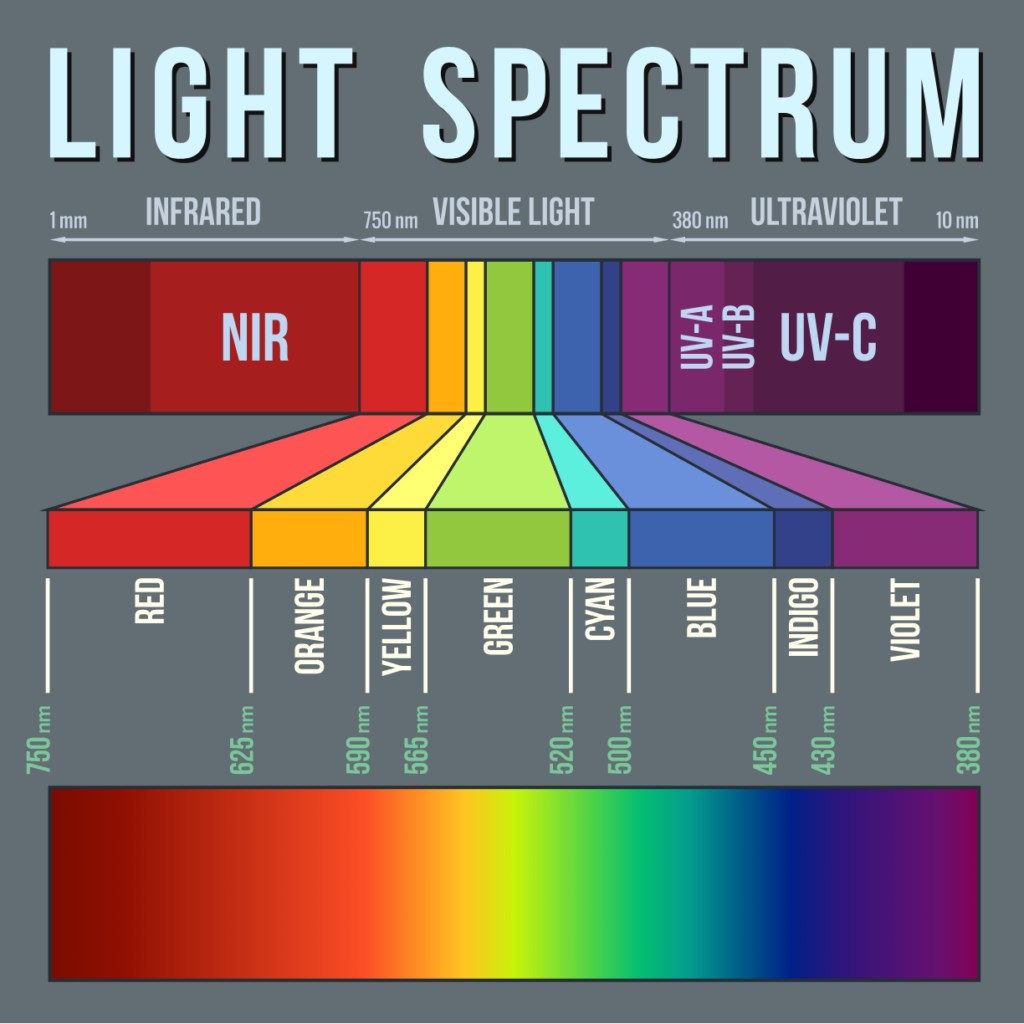
Red light is on the opposite end of the light spectrum. A 2012 study showed that exposure to only much longer wavelengths— 658 nm— for 30 minutes at night improved melatonin levels and sleep quality in athletes. 658 nm is inside the red light spectrum, which stretches from about 620 – 750 nm. To date, there are no studies showing that red light disrupts melatonin production.
Red Light Therapy Benefits
Photobiomodulation (PBM) uses near-infrared light, with wavelengths even longer than red light. PBM’s wavelengths increase blood flow, and are used by physical therapists to decrease inflammation in the body and promote healing. PBM has also played a therapeutic role in treating brain trauma, neurodegenerative disorders, cluster headaches, and psychiatric disorders including anxiety and treatment-resistant depression. In two studies, two weeks after a single treatment, patients grappling with both depression and anxiety found improvement or even remission of symptoms. In one study, PBM was also found to increase the blood flow in patients’ brains using a commercial near-infrared device.
Red Light Therapy at Home

A few months ago I hit a nasty period of insomnia that affected my performance at work. My boss suggested I try PBM, a field our organization is currently researching for its therapeutic benefits. I took a chance, and agreed to record my response to PBM in exchange for receiving a PBM device. The unit came in a tidy little box, and consisted of several red light appliques that look like butterfly bandages. I’ve used them every night for the past several months. Here are the results so far:
| PBM Usage | Time from end of treatment to sleep |
| Night 1 | 5 min |
| Night 2 | 10 min |
| Night 3 | 10 min |
| Etc. | 15 min |
| Last night | 10 min |
The first night I tried red light therapy, I fell asleep just five minutes after finishing treatment. The second and third nights it took slightly longer. Over the next few months of use, red light therapy put me to sleep about 80% of the time. When it works, it knocks me out within five to fifteen minutes. That’s amazing! The other 20%? Meh, it’s a work in progress. Sometimes, when I know my insomnia is particularly bad, I’ll combine red light therapy with another sleep aid like one milligram of melatonin. (Considering melatonin by itself doesn’t usually work for me, I still count this as a win for red light therapy.)
The medical consultant I’ve spoken with was extremely surprised that it worked for me, especially because the butterfly bandages were too large to place on my head (and too sticky to put in my hair) so I stuck it on my collarbone. But why would red light on my neck put me to sleep? He speculated that my results had something to do with a large artery running through the area. I tried placing the device on my stomach instead to see if it would work equally well, and it does not. My next question is whether it’s the red light putting me to sleep, or the heat put off by the device.
Does Red Light Cure Insomnia?
It’s not always easy to tell what’s causing sleeplessness, especially if there are several contributing factors. Heat waves and high temperatures can keep you awake, with or without sleep aids. However, red light therapy and Photobiomodulation (PBM) may help with insomnia due to physical or mental health problems and stress.
There is no conclusive data (yet) on whether or not red light therapy works as a cure for insomnia. However, it may still be worth trying for some individuals. As always, consult your doctor before going ahead with this or any other treatment.